Breastfeeding
Health professionals who provide infant feeding advice should have appropriate training and up-to-date knowledge on the benefits of breastfeeding. This helps ensure they can offer consistent, practical guidance and compassionate support – particularly for families who may experience challenges and need additional reassurance or assistance along the way.
The TEN STEPS to Successful Breastfeeding
World Health Organization. The TEN STEPS to Successful Breastfeeding [internet]. 2019 [cited Feb 2026], WHO.
This infographic outlines the World Health Organization and UNICEF Baby-Friendly Hospital Initiative Ten Steps to Successful Breastfeeding, summarising the evidence-based policies and practices recommended for maternity and newborn services to protect, promote and support breastfeeding within sustainable health systems.
Australian National Breastfeeding Strategy: 2019 and Beyond
Australian Government Department of Health. Australian National Breastfeeding Strategy: 2019 and Beyond. 2019 [cited Feb 2026]; Australian Government, Department of Health, Disability and Aging.
A national policy framework that guides coordinated action to protect, promote and support breastfeeding across Australia. It outlines priority areas, responsibilities and evidence-informed strategies for governments, health services and communities to improve breastfeeding initiation and duration, and to strengthen consistent, supportive care for families.
Infant Feeding and Parental Health
Australian Medical Association. Infant Feeding and Parental Health [internet]. 2017 [cited Feb 2026]; AMA.
Infant nutrition and early infant growth patterns lay the foundation for eating patterns, weight gain and reducing the risk of chronic conditions later in life. New parents should be supported to make decisions regarding the feeding of their infant, recognising that this will be influenced by numerous social, physiological and individual lifestyle factors.
Breastfeeding Position Statement
Australian Nursing & Midwifery Federation. Breastfeeding Position Statement. [internet]. 2024 [cited Feb 2026]; ANMF.
This position statement sets out the Australian Nursing and Midwifery Federation’s (ANMF) support for the Australian national breastfeeding strategy: 2019 and beyond and the responsibilities the ANMF considers nurses, midwives, health services and governments should meet to advance this strategy.
Infant Feeding – Nipple/Areola Eczema and/or Dermatitis
The Royal Women’s Hospital. Infant Feeding – Nipple/Areola Eczema and/or Dermatitis [internet]. 2024 [cited Feb 2026]; RWH.
Clinical guidelines for management of nipple/areola eczema and/or dermatitis. Skin conditions such as eczema or dermatitis may occur on the nipple and areola of pregnant and breastfeeding women. Management approaches are similar to eczema and dermatitis on other parts of the body.
Infant Feeding – Breast and Nipple Thrush
The Royal Women’s Hospital. Infant Feeding – Breast and Nipple Thrush [internet]. 2020 [cited Feb 2026]; RWH.
This guideline provides details for the signs, symptoms, and management of women with breast and nipple thrush. Breast and nipple thrush is the over-growth of Candida species, on the nipples and in breast ducts. Mother may describe burning, stinging nipple pain which continues during and after the feed.
Infant Feeding – Breastfeeding The Healthy Term Baby
The Royal Women’s Hospital. Infant Feeding – Breastfeeding The Healthy Term Baby [internet]. 2020 [cited Feb 2026]; RWH.
Breastfeeding of the healthy term baby should be supported by a baby-led, developmentally supportive approach. It is normal and physiologically beneficial for newborn babies to feed very frequently – usually 8-12 times in 24 hours. Cluster feeding and night feeds are normal and benefit both mother and baby.
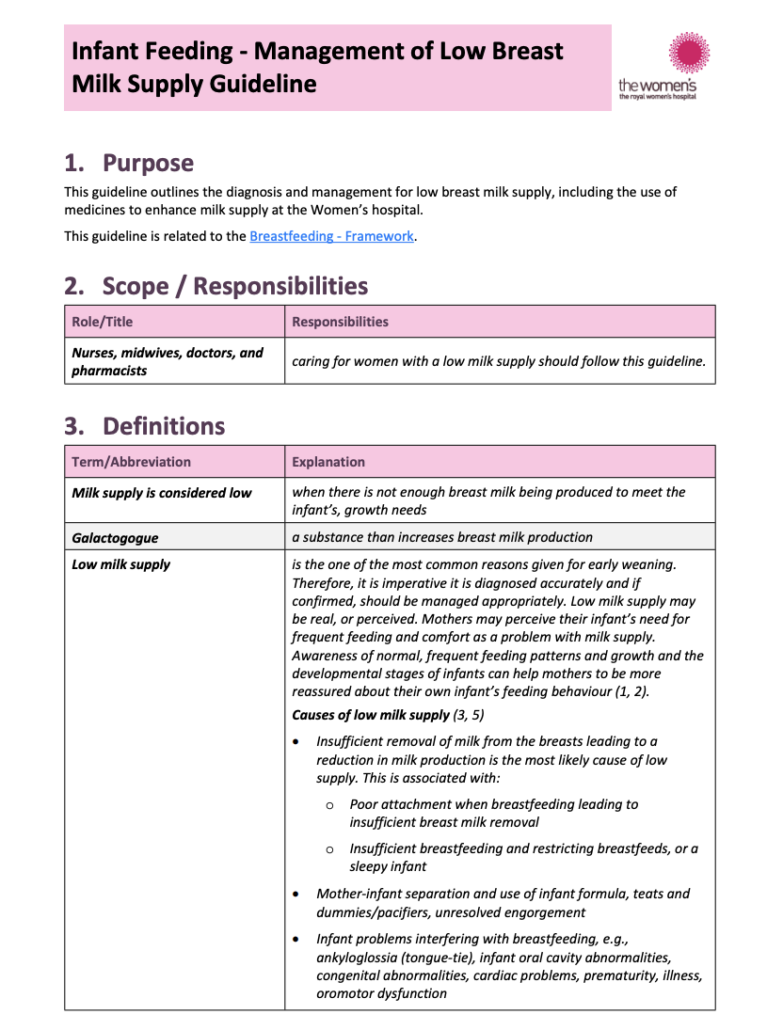
Infant Feeding – Management of Low Breast Milk Supply
The Royal Women’s Hospital. Infant Feeding – Management of Low Breast Milk Supply [internet]. 2020 [cited Feb 2026]; RWH.
Low milk supply is one of the most common reasons for early weaning. Insufficient removal of milk from the breasts leading to a reduction in milk production is the most likely
cause of low supply. Awareness of normal, frequent feeding patterns and growth and the developmental stages of infants can help mothers to be more reassured about their own infant’s feeding behaviour.
Infant Feeding – Mastitis And Breast Abscess
The Royal Women’s Hospital. Infant Feeding – Mastitis And Breast Abscess [internet]. 2020 [cited Feb 2026]; RWH.
Guidelines for pharmacological and non-pharmacological management of mastitis and breast abscess. Continuing to breastfeed and /or express breast milk is important for the management of mastitis. Diagnosis and treatment is important for health of mother and baby as delay in care may increase severity and risk of premature cessation of breastfeeding.
Infant Feeding – Nipple And Breast Pain In Lactation
The Royal Women’s Hospital. Infant Feeding – Nipple And Breast Pain In Lactation [internet]. 2020 [cited Feb 2026]; RWH.
Nipple pain and damage is one of the most common reasons for early cessation of breastfeeding. Most women experience nipple tenderness during the first week of establishing breastfeeding. Pain which is severe, persistent or occurs between feeds should be investigated. Nipple damage increases the risk of mastitis, formula supplementation and maternal anxiety.